Health
U.S. Vaccine Schedule Revamp Sparks Debate on Parental Authority

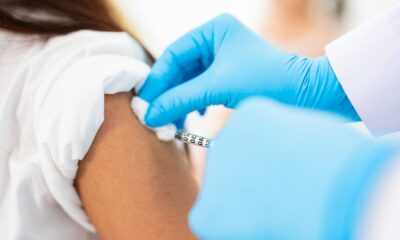
The recent changes to the U.S. pediatric vaccine schedule, implemented by Health and Human Services Secretary Robert F. Kennedy Jr., have ignited significant controversy. This overhaul demoted six vaccines from the routine recommendation category to what is termed “shared clinical decision-making” (SCDM). Critics argue that this shift implies these vaccines are optional or less effective than those typically recommended.
Public health experts largely agree on the safety and efficacy of these six vaccines, noting that the evidence supporting their use remains strong. Yet, while many in the health community criticize Kennedy’s approach, they may overlook a crucial aspect he has highlighted: vaccination decisions should involve patients and their parents, guided by clear communication from healthcare providers.
The principle of informed consent is foundational in medical practice, and vaccination should be no exception. In reality, many healthcare practitioners have approached informed consent as a routine procedure, often treating it as a formality rather than an ethical obligation. This has sometimes led to a perception that discussions around vaccination are more about compliance than genuine consent.
Historically, SCDM has been seen as a special category for vaccines with uncertain risk-benefit outcomes. For vaccines labeled as routine, the prevailing message has often been to proceed without discussion — an approach that prioritizes efficiency and vaccine uptake over patient autonomy. While this strategy has contributed to increased vaccination rates, it risks sidelining essential conversations about parental agency and informed consent.
The Centers for Disease Control and Prevention (CDC) has recommended a presumptive approach for pediatricians, advising healthcare providers to present vaccines as necessary without delving into discussions of choice. This method may enhance immediate compliance but fails to foster a long-term relationship of trust between parents and healthcare professionals.
Kennedy’s motivation in revising the pediatric vaccine schedule may not stem from a commitment to parental choice. Observers note that he appears more focused on undermining vaccine uptake. Nevertheless, his actions have sparked a necessary conversation about how vaccine discussions are framed.
Public health advocates are making notable communication errors in response to the new policy. By equating SCDM with “optional,” they risk reinforcing the narrative they oppose. Media coverage has often echoed this sentiment, leading the public to believe that the federal government considers many vaccines optional, primarily due to the language used by vaccine proponents.
Additionally, viewing parental choice as a threat grants Kennedy an unwarranted moral high ground. Instead of dismissing SCDM as a sign of weak evidence, public health professionals could redefine it as a legitimate aspect of informed consent, a vital component of ethical medical practice. Parents and patients have an inherent right to make informed decisions regarding medical interventions, including vaccinations.
While the new schedule may deter some hesitant parents from accepting every vaccine recommended by their pediatricians, it also respects their autonomy. Over time, this respect could foster a more positive relationship between parents and healthcare providers, potentially increasing vaccine acceptance.
The critical question now is whether public health professionals will embrace this shift or continue to resist it. The new pediatric vaccine schedule has explicitly highlighted parental agency in vaccination decisions. As the conversation evolves, public health must decide whether to support this change, emphasizing scientific evidence while allowing parents to guide their children’s healthcare choices.
In summary, the dialogue surrounding the pediatric vaccine schedule necessitates a reevaluation of how vaccination decisions are communicated. Emphasizing informed consent and allowing for shared decision-making can strengthen trust in vaccine science. Ultimately, this approach may lead to higher vaccination rates and better public health outcomes in the long run.
Peter M. Sandman, a retired expert in risk communication, advocates for a transformation in how vaccine discussions are conducted, suggesting that embracing parental choice could enhance both ethical standards and public confidence in vaccination.
-

 Science4 months ago
Science4 months agoNostradamus’ 2026 Predictions: Star Death and Dark Events Loom
-

 Science4 months ago
Science4 months agoBreakthroughs and Challenges Await Science in 2026
-

 Technology8 months ago
Technology8 months agoElectric Moto Influencer Surronster Arrested in Tijuana
-

 Technology5 months ago
Technology5 months agoOpenAI to Implement Age Verification for ChatGPT by December 2025
-
 Technology10 months ago
Technology10 months agoDiscover the Top 10 Calorie Counting Apps of 2025
-

 Health8 months ago
Health8 months agoBella Hadid Shares Health Update After Treatment for Lyme Disease
-

 Health8 months ago
Health8 months agoAnalysts Project Stronger Growth for Apple’s iPhone 17 Lineup
-

 Health8 months ago
Health8 months agoJapanese Study Finds Rose Oil Can Increase Brain Gray Matter
-

 Technology5 months ago
Technology5 months agoTop 10 Penny Stocks to Watch in 2026 for Strong Returns
-

 Science7 months ago
Science7 months agoStarship V3 Set for 2026 Launch After Successful Final Test of Version 2
-

 Technology7 months ago
Technology7 months agoInMotion Unveils P6 Electric Unicycle with 93 MPH Top Speed
-

 Technology2 months ago
Technology2 months agoNvidia GTC 2026: Major Announcements Expected for AI and Hardware