Health
Medicare Coverage of Ozempic to Revolutionize Weight Loss Options
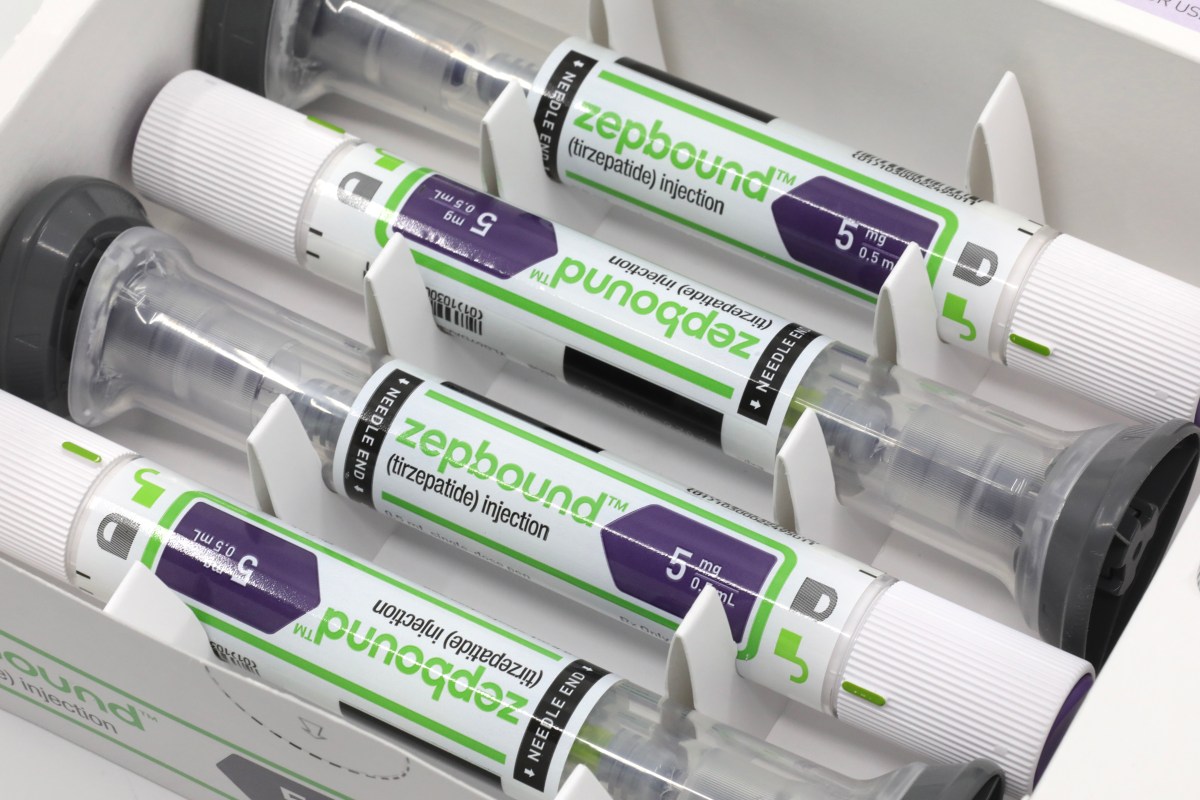
The CEO of Eli Lilly, Dave Ricks, announced that Medicare’s decision to cover Ozempic and other GLP-1 medications could significantly reshape weight loss treatment options in the United States. This development paves the way for Eli Lilly to launch its new obesity pill, orforglipron, potentially making effective weight loss solutions more accessible to millions.
According to the Centers for Disease Control and Prevention (CDC), from 2017 to 2020, 41.9 percent of U.S. adults were classified as obese, with approximately 9.2 percent fitting the criteria for severe obesity. GLP-1 medications, initially designed to treat type 2 diabetes, have emerged as transformative options for weight management. With Medicare’s new coverage policy, Eli Lilly anticipates a broader introduction of treatments for obesity.
As 2024 unfolds, Medicare will begin covering obesity medications for the first time, providing Eli Lilly an opportunity to launch its weight loss pill. Ricks noted that the company plans to have Medicare coverage “immediately following that launch, and that will change the game a bit too.” Currently, many patients pay out-of-pocket for competitor Novo Nordisk‘s GLP-1 product, Wegovy, which is priced at around $1,349 per month.
The anticipated launch of orforglipron in the second quarter of 2024 aligns with new pricing agreements between Eli Lilly, Novo Nordisk, and the administration of President Donald Trump. Under the new guidelines, Medicare patients could see their copay for injectable and oral GLP-1 medications reduced to approximately $50 per month. Ricks expressed optimism about the implications of this pricing structure, stating, “That opens up things pretty wide, and we’ll see where we can go from there.”
Ricks estimates that between 20 million and 30 million Medicare beneficiaries are affected by obesity, indicating that expanded coverage could substantially increase the pool of individuals eligible for treatment. The Trump administration had previously initiated a pilot program allowing state Medicaid programs and Medicare Part D plans to cover GLP-1 drugs for weight management.
Recent analyses highlight the financial implications of these treatments. A report from the Kaiser Family Foundation (KFF) revealed that Ozempic’s list price in the U.S. is around $936 per month, significantly higher than prices in many other countries. This raises questions about the sustainability of Medicare spending, which currently exceeds $35 billion annually on type 2 diabetes treatments, with a substantial portion allocated to GLP-1 medications.
In light of these developments, experts have shared their perspectives on the potential impact of GLP-1 medications. Alex Beene, a financial literacy instructor at the University of Tennessee at Martin, stated, “The effects of GLP-1 medication have been heavily touted in recent years… Lost is the incredible effect that could have on Medicare recipients, as excessive weight is a leading indicator of numerous other health complications for that age group.”
Financial advisor Drew Powers cautioned about the dual-edged nature of these treatments. He noted that while they could offer significant health benefits, the long-term financial implications for Medicare remain uncertain. “Will these drugs help patients lose weight and reverse their diabetes, thereby saving Medicare spending in the long run? Or will they be a life-long prescription that continues to cost an already-strained system?”
While the expanded coverage of GLP-1 medications holds promise for improving obesity rates in the U.S., healthcare professionals urge caution regarding potential side effects. These can include gastrointestinal issues, abdominal pain, and acid reflux. Beene emphasized the necessity for proper regulation and approval of these medications to ensure they mitigate side effects effectively.
As the landscape of weight loss treatment evolves, the implications of Medicare’s coverage decisions will be closely monitored by stakeholders across the healthcare spectrum. This shift not only highlights the growing recognition of obesity as a critical health issue but also poses significant questions about the future of healthcare funding and patient care in the United States.
-

 Science3 months ago
Science3 months agoNostradamus’ 2026 Predictions: Star Death and Dark Events Loom
-

 Science3 months ago
Science3 months agoBreakthroughs and Challenges Await Science in 2026
-

 Technology7 months ago
Technology7 months agoElectric Moto Influencer Surronster Arrested in Tijuana
-

 Technology4 months ago
Technology4 months agoOpenAI to Implement Age Verification for ChatGPT by December 2025
-
 Technology9 months ago
Technology9 months agoDiscover the Top 10 Calorie Counting Apps of 2025
-

 Health7 months ago
Health7 months agoBella Hadid Shares Health Update After Treatment for Lyme Disease
-

 Health7 months ago
Health7 months agoAnalysts Project Stronger Growth for Apple’s iPhone 17 Lineup
-

 Health7 months ago
Health7 months agoJapanese Study Finds Rose Oil Can Increase Brain Gray Matter
-

 Technology4 months ago
Technology4 months agoTop 10 Penny Stocks to Watch in 2026 for Strong Returns
-

 Science6 months ago
Science6 months agoStarship V3 Set for 2026 Launch After Successful Final Test of Version 2
-

 Technology1 month ago
Technology1 month agoNvidia GTC 2026: Major Announcements Expected for AI and Hardware
-

 Education7 months ago
Education7 months agoHarvard Secures Court Victory Over Federal Funding Cuts